We can now track biomarkers that have been found important in indicating current and future low back pain with more precision than ever
Most academic publications about lower back pain (LBP) will, at some point, feature a hand-wringing disclaimer something to the effect of “this is an extremely complicated problem, and isolating causes or indeed even quantifiable indicators of current pain is challenging at best”. It’s a fair point, and one that’s supported by the numbers; low back pain is the leading cause of disability worldwide (O'Sullivan et al., 2016), and roughly one third of patients who recover from an episode of low back pain will relapse within a year (Gustavo et al., 2017).
In the study Do Functional Tests Predict Low Back Pain (Takala et al., 2000), researchers worked with the Finnish Institute of Occupational Health to follow 430 workers in the Finnish forestry industry, 123 of whom suffered from low back pain and 307 of whom were nonsymptomatic. Subjects were put through a battery of tests designed to measure mobility and function (i.e. standing balance, foot reaction time, trunk ROM), and clinical tests (ie. SLR, sit-ups, and resisted hip flexion). Following initial selection, the workers were surveyed at the 1 and 2 year followups via a questionnaire. Their medical history and sick leave record requests in the elapsed year were also analyzed.
This study is noteworthy for a few reasons. Anecdotally, for MSK health studies that focus on range of motion (ROM)-related biomarkers it is relatively uncommon for subjects to be followed after the initial few tests. This study had a 24-month followup period that included not only subjective questionnaire responses but also objective clinical records (number of LBP-associated doctor’s visits, days of sick leave taken), providing valuable longitudinal data on the effectiveness of the functional capacity tests featured in the study. Days of sick leave in particular is highly relevant in a worker’s compensation context. Worth noting for those who may associate the forestry industry with highly demanding physical labor; 30% of workers were classified as having “light work” roles (office work and sedentary tasks) and 70% of workers were classified as having “moderately strenuous” (e.g. cleaning, various tasks at the paper machine, maintenance tasks). None were classified as performing heavy work.
Some key takeaways from the study:
Back pain affects everyone. The authors noted that the symptomatic and non-symptomatic groups had very similar distributions of sex, workload, stature and weight. Mean age differed by only 3 years between symptomatic and asymptomatic groups of men at the 2-year followup (39.4 years for those who stayed consistently pain free vs 42.4 years contracted pain). For women, the difference in average ages at 2-year follow-up between those who contracted pain vs those who did was even smaller (44.4 vs 43.2 years). Low back pain is by no means exclusive to elderly populations. Throughout the duration of the study, 22% of participants were diagnosed with a low back disorder and 17% of participants took sick leave due to a low back disorder.
The study measured and tracked trunk forward flexion with a tape measure. Lateral mobility during side bending was assessed using a rigid measuring tape, and pain was noted if reported (binary Yes/No). Straight leg raising was used for the provocation of back or leg pain. Functional activities performed included sit-up, resisted hip flexion, and passive back extension.
Differences between the contracted pain group, persistent pain group, pain-free group, and recovered group were analyzed, and variables statistically significant at P < 0.05 were identified. Researchers found that lumbar spine-pelvic movement ratio was associated with an increased number of medical consultations in the 2-year follow up period among male subjects. A shorter time until the first medical consultation was predicted by pain in side bending (P = 0.001) as well as during SLR (P = 0.005) for female subjects. In general, patients who were injured at the beginning of the study and eventually recovered showed better measures of balance and coordination during functional tests.
At the time of its publication in 2000, this study was noted for highlighting new clinical insights of pain and movement measures related to longitudinal occurrence and treatment of low back pain. At that time, mobile biomechanics technology to measure these key metrics with simultaneous tracking of a patient’s pain response during the movement did not exist in clinical settings. In fact, despite a boom in interest over the past 10 years in measuring human movement for sports and wellness, there has been limited integration of mobile biomechanics into musculoskeletal rehabilitation clinics.
The principle of the importance of tracking ROM and pain as biomarkers is timeless, and twenty-five years after the release of this study we now have tools to track pain during low back movement. The FIGUR8 biomotion Assessment Platform (bMAP) captures key biomechanical metrics, including pain, during a set of activities which are chosen specifically to provide the most clinically relevant information for treating persons with low back pain. The Low Back Assessment captures joint angles and muscle function in all 3 planes of motion during dynamic activities allowing clinicians to objectively quantify what our eyes see as the client moves, and also measure what our eyes can’t see. Tapping a button during data collection allows the clinician to identify the moment(s) in time that the patient reports pain throughout the movement trial. There is a clinical advantage of the FIGUR8 app’s ability to timestamp multiple pain points during each trial rather than a binary Yes/No (as recorded in this study, and as is common practice in PT clinics today). Each pain timestamp is associated with trunk ROM data, enabling clinicians to track the range of pain-free movement over multiple clinic visits.
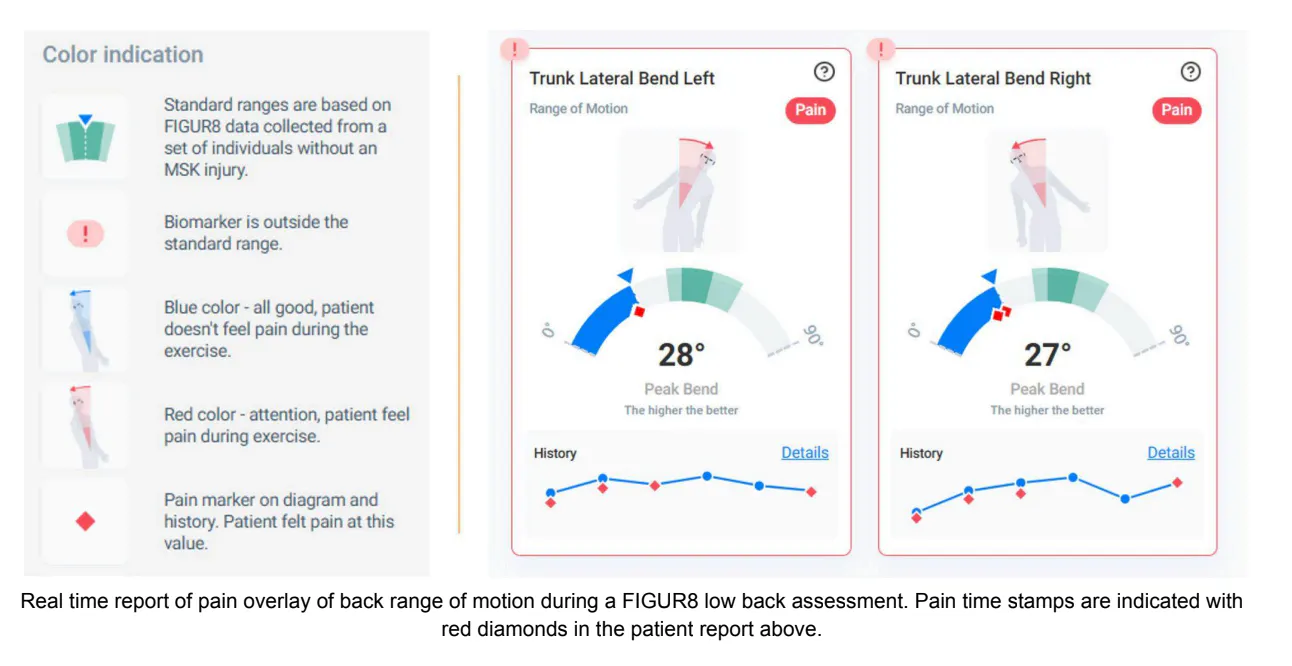
The study by Takala and Viikari-Juntura supports the need for application of newly available clinical biomechanics platforms that include a pain timestamp to assist in the treatment and research of low back patients. Further research on the relationship between low back pain and functional capacity is ongoing. To follow along with FIGUR8’s continuing research and learn more about how we’re bringing best-in-class biomechanics technology into the clinical environment, you can follow us at LinkedIn and connect with our team at info@figur8tech.com.
